Staph Infection Symptoms: Early Signs and Recognition
That red bump that won’t go away might be more than just a pimple. Staphylococcus bacteria live harmlessly on your skin most of the time, but when they slip inside through a cut or scratch, they can trigger infections that range from mildly annoying to genuinely dangerous. This guide walks through the early warning signs using guidance from medical institutions like the Mayo Clinic, Cleveland Clinic, and MedlinePlus, so you know what to watch for and when to take action.
Most common site: Skin ·
Typical skin signs: Boils, blisters, abscesses ·
Bacteria involved: Staphylococcus ·
Serious risks: Blood poisoning, toxic shock ·
Top sources: NHS, Mayo Clinic, CDC
Quick snapshot
- Skin infections most common per Mayo Clinic (Mayo Clinic)
- Symptoms include boils per CDC MedlinePlus (MedlinePlus)
- MRSA causes swollen bumps like pimples or spider bites (Mayo Clinic)
- Exact duration varies by individual case (Fronzuto Law)
- Regional symptom variations between UK and US not fully documented (Fronzuto Law)
- MRSA threat ongoing since 1960s (Mayo Clinic)
- Standard symptoms consistent across current sources (Mayo Clinic)
- Prompt medical attention prevents complications per MedlinePlus (MedlinePlus)
- Antibiotic treatment usually resolves mild cases (Mayo Clinic)
The table below summarizes key facts about staph infections, drawing from multiple medical authorities.
| Category | Details |
|---|---|
| Primary bacteria | Staphylococcus aureus |
| Top symptom | Skin boils and abscesses |
| Common location | Skin and nose |
| MRSA variant | Methicillin-resistant strain |
| Fever threshold | 38°C or higher |
| Diagnosis (mild) | Visual inspection |
| Diagnosis (severe) | Blood tests, cultures, imaging |
| Complications | Sepsis, endocarditis, osteomyelitis |
How do you tell if you got a staph infection?
Staph bacteria cause distinct changes in the skin that most healthcare providers can identify through a physical exam. The Mayo Clinic notes that serious skin symptoms include discolored, swollen, warm, painful skin, blisters that break leaving a raw surface, fever, chills, and malaise (Mayo Clinic). Knowing these signs matters because early detection prevents the infection from spreading deeper into the body.
Skin changes
- Red, swollen, or darkened skin around a wound or break
- Skin that feels warm to the touch
- Yellow-colored scabs or crusty patches
- Weeping or fluid leaking from the affected area
Pain and swelling
The Cleveland Clinic describes staph skin symptoms as swollen, warm, red, painful, pus-filled, crusty, itchy, and sometimes peeling (Cleveland Clinic). Pain that feels out of proportion to the visible wound is a red flag—staph infections often create deep tissue involvement that isn’t obvious from the surface. The infected area may feel firm or mushy underneath, and pressing on it often causes significant discomfort.
When to seek help
Healthdirect, an Australian government health service, identifies a fever of 38°C or higher as a key symptom requiring urgent attention (healthdirect). If a skin lesion is accompanied by fever, chills, or general malaise, it’s time to see a doctor. Wounds that don’t show signs of healing within a few days, or that suddenly worsen after initially improving, also warrant professional evaluation.
A delay in diagnosing and treating staph infections can be fatal. Medical malpractice analysis from Fronzuto Law Group confirms the stakes are highest when the infection spreads to the bloodstream before treatment begins (Fronzuto Law).
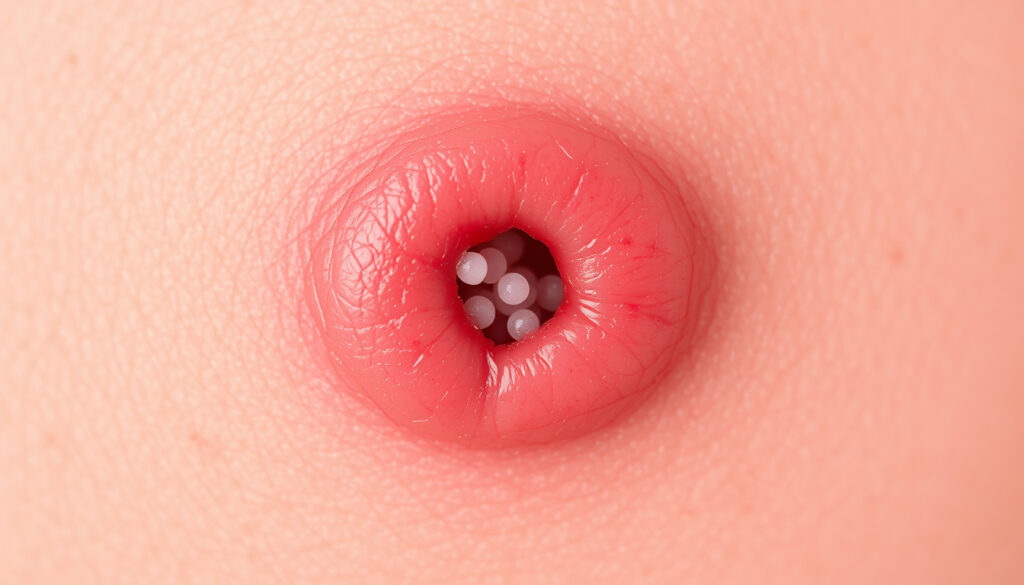
What does the first stage of a staph infection look like?
Early staph skin infections often resemble common skin problems, which is why they get dismissed or misdiagnosed. HealthPartners explains that early staph skin infections look like pimples or blisters, swollen and red and warm, and are common on the face, mouth, and nose (HealthPartners). This deceptive similarity to everyday blemishes means the window for quick treatment often closes while people wait to see if the “pimple” resolves on its own.
Early skin signs
- A small red bump that may resemble a pimple
- Localized warmth around the bump
- Tenderness when touched
- Potential development of a white or yellow center
Red lump or bump
Mayo Clinic identifies swollen, painful bumps that look like pimples or spider bites as an early symptom of skin infections caused by staph bacteria, including MRSA (Mayo Clinic). The key difference from a normal pimple is that these bumps tend to be larger, more painful, and don’t respond to typical acne treatments. Medical News Today notes that MRSA lesions specifically show red, swollen, warm, painful areas that may leak pus (Medical News Today).
Progression to boil
Without treatment, that small bump evolves into something more serious. Mayo Clinic describes common skin staph infections including impetigo with sores on the face that burst and leave yellow crust, folliculitis with pus-filled itchy bumps, and boils or furuncles that form deep pus pockets (Mayo Clinic). The progression from pimple-like bump to full-blown boil can happen within days, especially if the area is irritated or covered.
Healthline describes CA-MRSA causing swollen painful bumps resembling spider bites or pimples with a yellow or white center (Healthline). This visual clue—a central head filled with pus—is one of the most reliable indicators separating staph from a routine skin irritation.
What are the causes of Staphylococcus infection?
Staph bacteria are opportunistic—they cause problems only when they find a way inside the body. Mayo Clinic notes that staph bacteria are often harmless on the skin or in the nose but infect damaged skin such as from eczema, bites, or injections (Mayo Clinic). Understanding these entry points helps you assess your own risk and take targeted precautions.
Bacteria entry points
- Cuts, scrapes, or surgical wounds
- Bug bites or animal scratches
- Injection sites (particularly IV drug use)
- Skin conditions like eczema or dermatitis
- Burns or thermal injuries
Risk factors
Mayo Clinic identifies several risk factors: chronic skin disease, burns, wounds, surgery, and injections (Mayo Clinic). People with weakened immune systems, those hospitalized, and residents of long-term care facilities face elevated risk. Athletes in close-contact sports, caregivers, and children in daycare settings also have higher exposure rates.
Common triggers
The infection often begins with a minor skin break that goes unnoticed or untreated. Impetigo, highly contagious and caused by staph, spreads easily through direct contact (HealthPartners). Crowded environments, poor hygiene practices, and shared equipment or towels create ideal conditions for transmission. Hospital settings present specific risks through post-surgical wound contamination and poor sanitation (David Kates Law).
The implication: staph exploits the smallest breaks in skin integrity, making awareness of cuts, abrasions, and skin conditions your first line of defense.
Where is the most common place to get a staph infection?
The skin is the body’s first defense and its most frequent site of staph invasion. Mayo Clinic confirms that skin infections are the most common manifestation of staph bacteria (Mayo Clinic). Beyond the skin surface, these bacteria commonly colonize the nose, creating a reservoir for self-infection whenever the carrier touches a skin break.
Skin infections
CBS News notes that staph infections are common on hair-covered areas like the neck, groin, and armpit (CBS News). Mayo Clinic’s verified data confirms that boils and furuncles commonly appear under the arms, in the groin, and on the buttocks (Mayo Clinic). These warm, moist areas provide ideal conditions for bacterial growth and are frequently subject to friction and minor trauma.
Nose carriage
The nose harbors staph bacteria in a significant percentage of the population without causing any symptoms. MedlinePlus confirms that staph bacteria commonly live on the skin or in the nose (Mayo Clinic). This asymptomatic carriage means people can spread the bacteria to others or infect themselves without realizing it. Healthcare workers, dialysis patients, and people with diabetes face higher rates of nasal colonization.
Other body sites
While skin and nasal colonization represent the majority of cases, staph can affect internal sites when the bacteria enter the bloodstream. Mayo Clinic notes that staph bacteremia can lead to sepsis and septic shock if untreated (Mayo Clinic). Joint replacements, artificial heart valves, and other medical devices provide surfaces where staph can form stubborn biofilms that are difficult to eradicate.
What this means: the same bacteria colonizing your nose without symptoms can become life-threatening if it breaches damaged skin anywhere on your body.
What is the fastest way to cure a staph infection?
Treatment speed depends on infection severity, and getting it right matters more than getting it fast. MedlinePlus states that staph diagnosis involves physical examination, often visual for skin cases, with cultures used for other types of infections (MedlinePlus). The treatment approach that works fastest is the one that targets the specific type of staph involved and the location of the infection.
Medical treatments
- Antibiotics prescribed based on culture results
- Drainage of abscesses by a medical professional
- Wound care and dressing changes
- IV antibiotics for severe or bloodstream infections
- Monitoring for complications in high-risk patients
Home care limits
Mayo Clinic notes that MRSA, a methicillin-resistant staph variant, is common in hospitals and the community, making some standard antibiotics ineffective (Mayo Clinic). At-home care like warm compresses and over-the-counter pain relievers can ease symptoms but cannot cure the infection. Attempting to drain an abscess yourself risks spreading the bacteria deeper into tissue or the bloodstream.
Prevention basics
Healthdirect recommends keeping wounds clean and covered, washing hands frequently, and avoiding sharing personal items like towels or razors (healthdirect). These simple habits significantly reduce both your risk of contracting a staph infection and your likelihood of spreading one to others. People with recurrent staph infections may need nasal antibiotic ointments or bleach baths under medical supervision.
Upsides
- Most skin staph infections respond well to antibiotics when caught early
- Visual diagnosis often sufficient for mild cases, enabling rapid treatment
- Good hygiene practices effectively prevent most transmissions
- Abscess drainage provides immediate symptom relief
Downsides
- MRSA requires different antibiotics, complicating initial treatment
- Misdiagnosis or delay can allow spread to bloodstream
- Recurrent infections common in carriers
- Severe cases need hospitalization and IV therapy
What experts say
Swollen, painful bumps that look like pimples or spider bites are an early symptom of skin infections caused by staph bacteria, including MRSA.
— Mayo Clinic (Medical Institution)
Delay in diagnosis and treatment, the two main allegations for most medical malpractice actions, can be fatal for staph infections.
— Fronzuto Law Group (Medical Malpractice Analysis)
Staph bacteria are often harmless on the skin or nose but infect damaged skin such as from eczema, bites, or injections.
— Mayo Clinic (Medical Institution)
Related reading: Peripheral Nervous System Functions & Disorders · Infrared Sauna Benefits Mayo Clinic
Staph infections often resemble other bacterial skin issues such as impetigo first signs pictures, which display characteristic red sores and honey-crusted blisters in early stages.
Frequently asked questions
What are the five signs of an infection?
The classic signs are redness, warmth, swelling, pain, and pus or drainage from the wound site. A fever above 38°C may also develop if the infection spreads. Cleveland Clinic lists swollen, warm, red, painful, and pus-filled skin as key symptoms of staph infections. Any combination of these warrants medical evaluation.
What can be mistaken for staph infection?
HealthPartners notes that early MRSA bumps closely resemble spider bites or pimples, leading to misidentification. Impetigo can be confused with cold sores or allergic reactions. Folliculitis may resemble acne or razor burn. Fungal infections like athlete’s foot sometimes present similarly to staph between the toes. When in doubt, a medical provider can perform a quick culture to confirm the diagnosis.
How long does staph last untreated?
The duration varies significantly based on infection type, location, and individual health factors. Mild skin infections may persist for weeks or months without treatment, while severe bloodstream infections can become life-threatening within days. Mayo Clinic warns that untreated staph bacteremia can progress to sepsis and septic shock, making any persistent or worsening skin lesion a reason to seek care promptly.
Can staph infection kill you?
Yes, untreated staph infections can be fatal. Mayo Clinic confirms that staph bacteremia can lead to sepsis and septic shock if left untreated. The infection can also cause serious complications including staphylococcal pneumonia, endocarditis, osteomyelitis, septic arthritis, and thrombophlebitis. Prompt treatment dramatically improves outcomes for most otherwise healthy individuals.
What are different types of staph infections?
Mayo Clinic lists common skin staph infections including impetigo with yellow-crusted sores, folliculitis with pus-filled itchy bumps, and boils or furuncles as deep pus pockets. Other types include cellulitis (hot swollen red under-skin), staphylococcal scalded skin syndrome (affecting children under 6 with skin-peeling like a burn), and MRSA, the antibiotic-resistant variant. Internal infections can affect bones, joints, heart valves, and lungs.
The pattern is clear: staph infections exploit small openings in your defenses and exploit them fast. For patients with a new skin lesion that looks wrong or feels painful beyond what it appears, waiting is the riskier choice. Early visual recognition saves lives, and the cost of a doctor’s visit is nothing compared to the cost of treating sepsis.